How Technology Is Improving Remote Monitoring for LVAD Patients
Left Ventricular Assist Devices (LVADs) are mechanical circulatory support systems used to assist patients with advanced heart failure. These devices pump blood from the left ventricle to the aorta, supplementing cardiac output when the heart cannot meet physiological demands. As LVAD therapy has become more prevalent, remote monitoring technology has emerged as a critical component of post‑implant care.
Remote monitoring encompasses a suite of digital tools and data transmission methods that allow clinicians to track device performance, patient physiological status, and indicators of emerging complications without requiring in‑person visits. The combination of implantable hardware, wearable adjuncts, patient interfaces, and clinical dashboards has driven a paradigm shift in LVAD management, improving outcomes, reducing unnecessary hospitalizations, and enhancing patient quality of life.
This article provides an expert‑level review of how technology is improving remote monitoring for LVAD patients, with a practical focus on clinical implementation, patient support systems, and specialized patient needs—including adaptive apparel such as the HeartMate tank top and considerations in lvad clothing for patients to support device use and daily life.
Fundamentals of LVAD Remote Monitoring
What Remote Monitoring Means in LVAD Care
Remote monitoring refers to continuous or scheduled electronic collection and transmission of data from an LVAD system and associated biometric sensors to a clinical care team. This typically includes:
-
Device operational parameters (e.g., pump speed, power, calculated flow)
-
Physiological metrics (e.g., heart rate, blood pressure, activity levels)
-
Alerts and event notifications indicating potential device or patient status changes
Data can be transmitted via cellular, Wi‑Fi, or Bluetooth connections. Clinicians receive data through secured cloud‑based platforms or vendor‑specific portals, allowing for timely analysis.
Why Remote Monitoring Matters
LVAD patients often face complex clinical trajectories, including risks of thrombosis, infection, and right heart failure. Traditional follow‑up intervals—often every few weeks or months—are insufficient to capture short‑term hemodynamic changes that precede clinical decompensation. Remote monitoring bridges that gap by enabling:
-
Early detection of adverse events
-
Reduced emergency hospitalizations
-
Optimized individualized therapy adjustments
-
Enhanced patient engagement in self‑management
Industry standards emphasize prompt intervention upon detection of abnormal LVAD trends as a strategy to improve survival and reduce morbidity.
Core Technologies in Remote LVAD Monitoring
Implantable Sensors and Device Telemetry
Modern LVADs incorporate internal sensors that measure pump function variables. These sensors provide:
-
Pump speed and power consumption
-
Estimated flow calculations
-
Motor temperature and vibration data
Telemetry modules transmit these data to home units or wireless hubs. Clinicians interpret trends to detect early signs of pump dysfunction, hemolysis, or obstructions in flow paths.
Wearable and Peripheral Monitoring Devices
Supplemental wearable devices enhance patient monitoring by capturing biometric and activity data:
-
Continuous heart rate monitors
-
Ambulatory blood pressure monitors
-
Physical activity trackers
Correlation between physiological data and LVAD performance offers deeper insights into patient status, particularly for symptoms like fatigue or dizziness that may indicate outflow graft obstruction or arrhythmias.
Home Data Hubs and Secure Platforms
These include:
-
Dedicated home communication units paired with the LVAD
-
Smartphone applications that collect and relay data
-
Cloud‑based clinician dashboards
Security protocols ensure encrypted transmission and storage, aligning with healthcare privacy standards such as those defined by national regulatory agencies.
Clinical Impact and Real‑World Applications
Early Detection and Intervention
Remote LVAD monitoring enables clinicians to identify:
-
Abnormal power spikes indicating potential thrombosis
-
Downward trends in estimated flow suggesting dehydration or hypovolemia
-
Arrhythmic patterns or excessive variability prompting adjustments
In practice, care teams can adjust anticoagulation regimens, recommend fluid balance management, or schedule earlier in‑clinic evaluations based on remote data, often before symptoms worsen.
Reduced Hospital Utilization
Large cohort analyses by major cardiac centers show reductions in readmission rates for LVAD patients enrolled in structured remote monitoring programs. These programs enhance longitudinal assessment and decrease reliance on emergent care pathways.
Patient Quality of Life
Remote monitoring reduces the need for frequent travel to specialized centers, which can be burdensome for patients with limited mobility. By enabling real‑time supervision and timely intervention, patients spend more time at home and maintain higher functional autonomy.
Integrating Patient‑Centered Supports: Apparel and Lifestyle Considerations
LVAD therapy presents unique challenges in daily living, particularly related to device components such as drivelines and controller housings. Appropriate clothing and accessories support comfort, functionality, and safety.
Apparel Designed for LVAD Patients
Clothing specifically engineered for LVAD patients helps protect device components, reduce irritation, and facilitate discreet management in public or private settings. Examples include garments with strategic access points for drivelines, reinforced pockets for controllers, and fabric choices that minimize friction.
Specialized Tops for LVAD Comfort
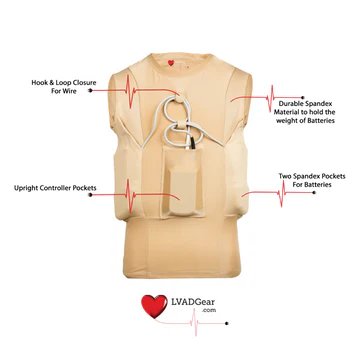
The HeartMate tank top exemplifies adaptive garments that accommodate LVAD components while promoting comfort and mobility. These tank tops often feature:
-
Soft, breathable fabrics
-
Secure storage for device controllers
-
Easy access for dressing and wound care
-
Enhanced comfort during physical activity
Broader Clothing Guidance for LVAD Patients
Comprehensive lvad clothing for patients resources provide guidance on selecting garments that:
-
Reduce pressure on exit sites
-
Allow proper routing of drivelines
-
Support temperature regulation
-
Facilitate attachments for remote monitoring accessories
Patient education on clothing selection is a practical extension of clinical care, minimizing skin irritation, infection risk, and interference with device function.
Expert Insights and Best Practices
Structured Monitoring Protocols
Clinics with well‑developed remote monitoring programs establish standardized:
-
Data review intervals
-
Alert thresholds
-
Intervention protocols
Regular interdisciplinary team meetings ensure that cardiologists, LVAD coordinators, and nurses interpret trends consistently.
Patient Training and Engagement
Effective remote monitoring depends on patient competence with technologies. Best practices include:
-
Hands‑on training at device discharge
-
Instructional materials addressing common technical issues
-
Routine competency assessments
Patients and caregivers who understand device data and alert significance are better partners in long‑term management.
Common Mistakes and Misconceptions
Over‑Reliance on Raw Data Without Clinical Context
Remote monitoring data must be interpreted by trained clinicians. Raw trends without clinical correlation can lead to inappropriate interventions.
Assuming All Alerts Require Urgent In‑Person Evaluation
Not all device anomalies necessitate emergency care. Triage protocols distinguish between actionable trends and benign variations.
Neglecting Patient Comfort and Practicality
Remote monitoring strategies should integrate patient lifestyle considerations, including apparel and ergonomic device management, to maximize adherence and minimize device‑related complications.
Conclusion
Technological advances in remote monitoring fundamentally reshape LVAD patient care. By leveraging implantable sensor data, wearable monitors, and secure communication platforms, clinicians can detect early signs of complications, tailor therapy, and reduce dependence on traditional in‑person visits.
Integrating patient‑centered supports, including adaptive apparel such as the HeartMate tank top and comprehensive guidance on lvad clothing for patients, underscores the importance of addressing both clinical and practical aspects of LVAD therapy. Expert implementation of structured remote monitoring protocols enhances outcomes, increases patient autonomy, and represents a benchmark for advanced cardiovascular device management.
FAQs
What is an LVAD and how does it work?
An LVAD is a surgically implanted pump that assists the left ventricle in circulating blood. It draws blood from the heart’s left ventricle and delivers it to the aorta under controlled speed and flow, reducing the workload on the failing heart.
How does remote monitoring enhance LVAD care?
Remote monitoring allows clinicians to receive device performance and patient physiological data on an ongoing basis. This enables early detection of issues, individualized therapy adjustments, and reduced need for frequent clinic visits.
What technologies are used to collect remote data?
Technologies include implantable device sensors, wearable biometric monitors, home data hubs, smartphone interfaces, and secure cloud platforms for clinician access.
Are there standards for remote monitoring in LVAD patients?
Yes, professional societies and device manufacturers define performance metric thresholds, alert protocols, and secure communication standards to guide remote monitoring practices.
Can remote monitoring prevent hospitalizations?
Evidence from clinical programs indicates that structured remote monitoring can reduce unnecessary hospital admissions by identifying and addressing patient needs before they escalate.
What role does patient‑centered clothing play?
Adaptive clothing, including LVAD‑specific tops and garments, accommodates device components, enhances comfort, protects exit sites, and supports daily mobility and activity.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Jeux
- Gardening
- Health
- Domicile
- Literature
- Music
- Networking
- Autre
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness



